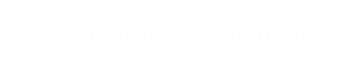
Knee Treatments
Knee Anatomy
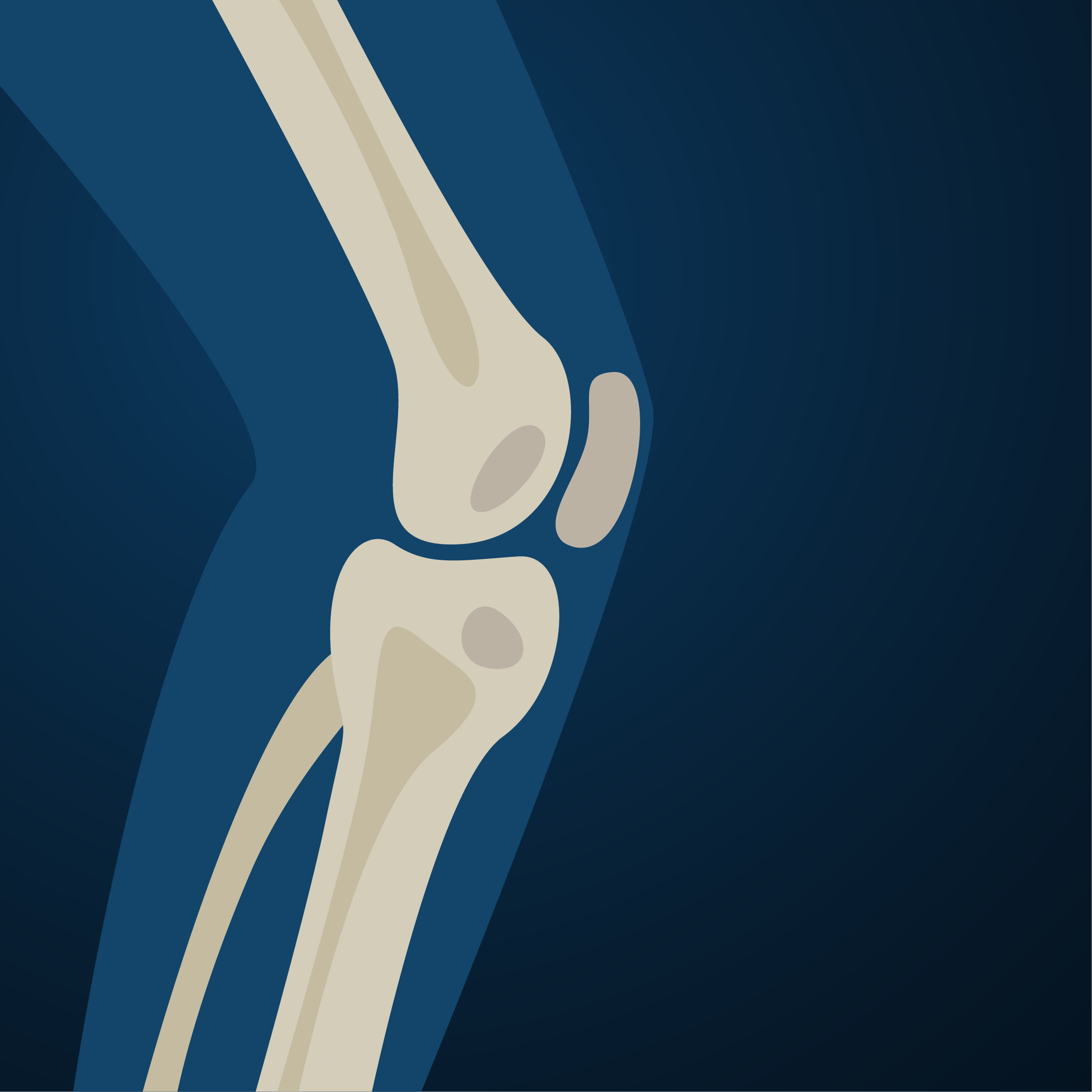
The knee is the largest joint in the body and functions as a complex hinge connecting the thigh bone (femur) to the shin bone (tibia). It also includes the smaller fibula bone in the lower leg. In addition to bending and straightening the leg, the knee allows limited rotation and side movement. Several key structures surround and support the joint, including ligaments, tendons, and muscles.
The medial and lateral collateral ligaments, along with the anterior and posterior cruciate ligaments, stabilize the joint. Meanwhile, the quadriceps and hamstring muscles enable movement and strength.
The knee joint is covered with hyaline cartilage, which cushions the joint and helps it move smoothly. Two shock-absorbing menisci add extra protection between the bones. Furthermore, the synovial membrane produces synovial fluid, which lubricates the joint and reduces friction.
Common knee injuries include ligament sprains or tears, meniscus tears, and patellar dislocations. Depending on the injury’s severity, treatment options may include physical therapy, rest, or surgery. With appropriate care, many patients recover well and regain full mobility.
Knee Pain
Knee pain can significantly interfere with daily life. Dr. Jones provides both non-surgical and surgical treatment options designed to address knee pain efficiently. He has extensive experience helping patients in Colorado Springs recover from knee injuries through tailored care and guidance.
Knee Treatments and Specialties
ACL Tears
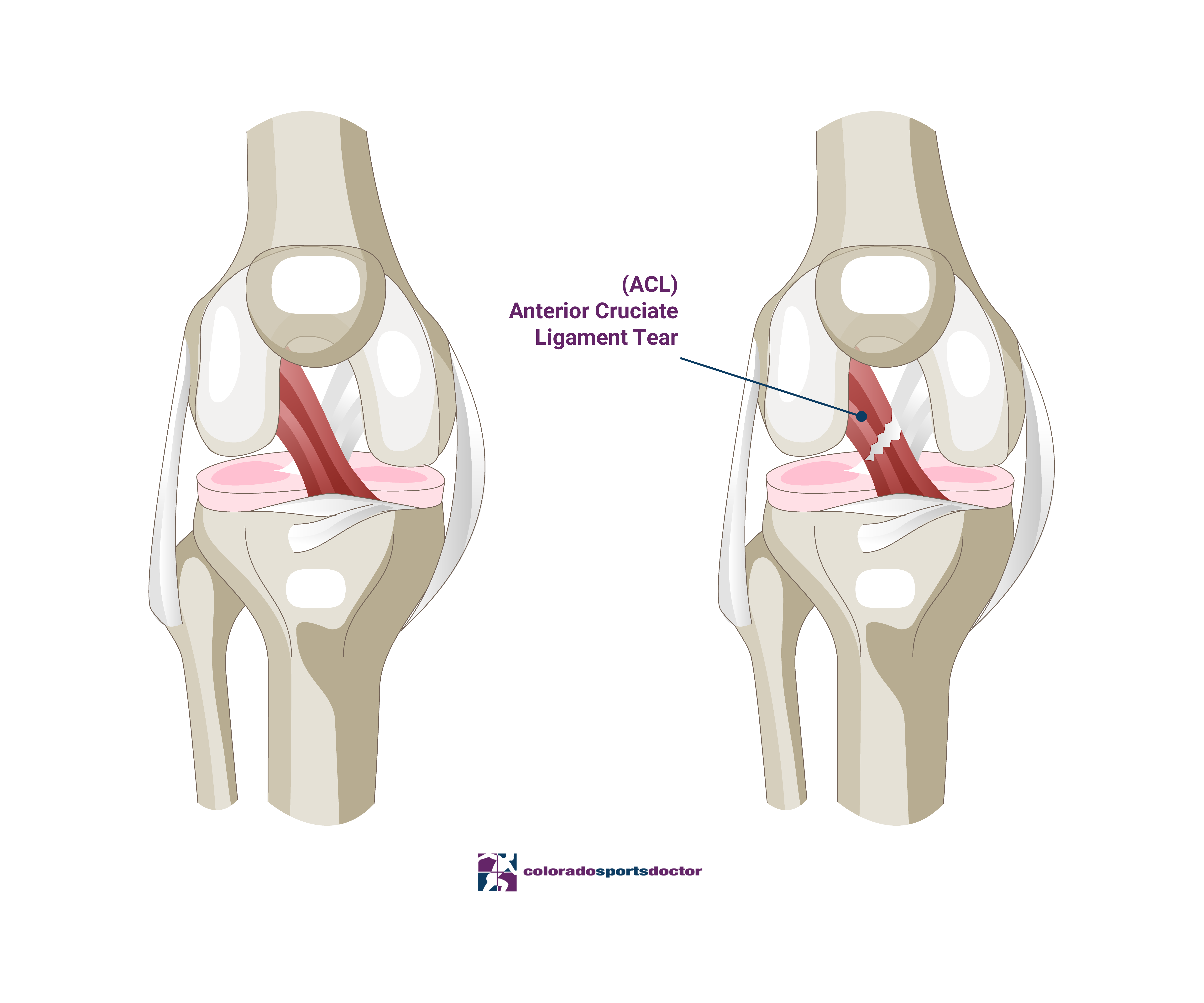
An anterior cruciate ligament (ACL) tear commonly occurs during high-impact sports or activities that involve twisting motions. The ACL, one of the four main ligaments in the knee, stabilizes the joint during pivoting and quick direction changes. When the ligament tears, pain, swelling, and instability usually follow.
Treatment depends on the severity of the tear and a patient’s activity level. In mild cases, rest and physical therapy may allow the ligament to heal. However, surgery might be necessary in more severe cases to repair or reconstruct the ligament.
Recovery time varies depending on the injury’s extent and adherence to rehabilitation. With appropriate treatment, many people regain strength and return to their normal activity levels.
In addition, prevention plays an important role. Warming up properly, wearing supportive shoes, and strengthening muscles around the knee can reduce the risk of ACL injuries.
Cartilage Injuries
Cartilage injuries involve damage to the articular cartilage, the smooth, durable surface covering bone ends in the joint. This cartilage allows for frictionless motion during walking, running, and other activities.
However, degeneration from aging, excessive weight, or repetitive injuries can damage this tissue. Symptoms include pain during weight-bearing, swelling, or sensations of catching and locking in the knee. Because these symptoms can vary, accurate diagnosis often requires imaging or arthroscopy.
Treatment aims to relieve pain and restore knee function. Options may include chondroplasty to remove loose cartilage, microfracture to stimulate healing, osteochondral grafts to replace damaged tissue, and autologous chondrocyte implantation (ACI) to repair cartilage using the patient’s own cells. Selecting the right approach depends on the injury’s size, location, and severity.
Meniscus Injuries
The meniscus is a crescent-shaped structure inside the knee. It distributes weight evenly and prevents the femur and tibia from rubbing together. The medial meniscus sits on the inner knee, while the lateral one lies on the outer side.
Meniscus tears are common among athletes and older adults. They usually occur after twisting or turning the knee suddenly. Symptoms include pain, swelling, locking, and difficulty straightening the leg.
Conservative care often includes rest, ice, compression, elevation, and physical therapy to restore strength and flexibility. In more severe cases, Dr. Jones may recommend surgery to repair or remove the damaged tissue.
Chondromalacia
Chondromalacia affects the cartilage beneath the kneecap (patella). This cartilage allows the joint to move smoothly by reducing friction. When it softens or breaks down, patients experience pain and discomfort.
The condition is more common in young adults and athletes who place repeated stress on their knees, such as runners or jumpers. Symptoms include dull, aching pain when bending or straightening the leg, and sometimes a cracking or popping sound.
Treatment may include rest, ice, physical therapy, and platelet-rich plasma (PRP) injections. In more advanced cases, surgery may be necessary to smooth or repair damaged cartilage.
Cartilage Restoration
Cartilage restoration procedures aim to repair damaged cartilage and restore smooth joint movement. Damage may result from injury or degenerative conditions such as osteoarthritis.
Several treatment options are available, including matrix-induced autologous chondrocyte implantation (MACI), osteochondral allografts (OCA), stem cell therapy, and platelet-rich plasma (PRP). These methods encourage the growth of new cartilage and improve joint function.
Recovery varies depending on the treatment and patient condition. Rehabilitation and gradual return to activity are key factors in long-term success. Advances in medical technology continue to improve outcomes for cartilage restoration procedures.
Platelet-Rich Plasma Therapy (PRP)
Platelet-rich plasma (PRP) therapy uses a patient’s own platelets to promote healing in damaged or inflamed tissues. A small blood sample is processed in a centrifuge to separate the plasma and concentrate the platelets.
These platelets contain growth factors that help reduce inflammation and support tissue repair. The PRP solution is injected directly into the knee joint to relieve pain and aid recovery, particularly for conditions such as osteoarthritis and ligament injuries.
This minimally invasive treatment is typically performed in an outpatient setting. Multiple sessions may be required for the best results. Recovery times are shorter than those for surgery, and many patients notice improvement in pain and function within weeks to months.
Bone Marrow Concentrate Therapy (BMAC)
Bone marrow concentrate (BMAC) therapy is an advanced biologic treatment used to enhance tissue healing. Dr. Jones, a fellowship-trained orthopedic surgeon, uses these therapies for patients whose conditions do not respond to traditional surgical or non-surgical options.
BMAC and PRP therapies can serve as standalone treatments or be combined with surgery. They are used for conditions such as tendon injuries, partial rotator cuff tears, ligament damage, and early osteoarthritis. Both treatments help reduce inflammation and support the body’s natural healing response.
Although some insurers still classify these therapies as experimental, Dr. Jones continues to refine and evaluate his treatment protocols to ensure safe, effective, and affordable care for patients.
"*" indicates required fields
Our Location
Dr. Christopher K. Jones, MD
4110 Briargate Parkway #300
Colorado Springs, Colorado 80920
Hours
Monday: 9am-5pm
Thursday 9am-5pm
Friday 9am-5pm